Understanding Your Spine: A Guide to Back Anatomy and Pain
If you're experiencing back pain, you're not alone. Back pain affects nearly half of all people in their 50s and 60s, making it one of the most common health concerns during this stage of life. Understanding the basic anatomy of your spine and how it changes with age can help you make sense of your symptoms and have more informed conversations with your healthcare provider.
The Building Blocks of Your Spine
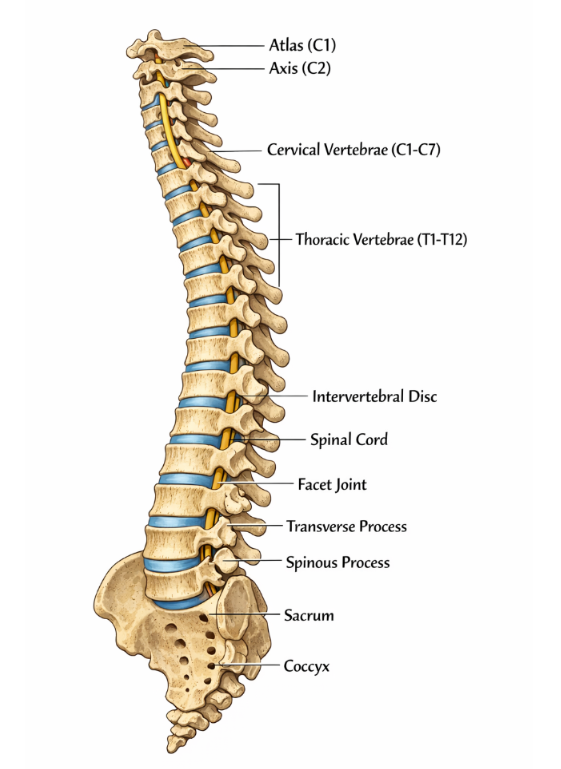
Think of your spine as a stack of building blocks called vertebrae. You have 24 movable vertebrae in your spine: seven in your neck (cervical spine), twelve in your mid-back (thoracic spine), and five in your lower back (lumbar spine). Below these sits your sacrum, a triangular bone that connects to your pelvis. Between each vertebra sits a cushion called an intervertebral disc. These discs are remarkable structures—they're about 70-80% water and act like shock absorbers for your spine. Each disc has a tough outer ring (the annulus fibrosus) and a gel-like center (the nucleus pulposus). When you bend, twist, or lift something, these discs compress and expand, distributing the forces evenly throughout your spine. Behind each vertebra are two small joints called facet joints. These joints allow your spine to bend and twist while keeping it stable. Surrounding all of these structures are ligaments (tough bands of tissue that connect bones), muscles, and nerves that work together to support your body and allow movement.
Figure 1- An illustration of the spine
How Your Spine Changes Over Time
As we age, our spines undergo natural changes that can contribute to pain. These changes often begin as early as our 30s and 40s, but become more noticeable after age 50, particularly for women. The most common change involves the intervertebral discs. Over time, these discs lose water content and become less flexible—imagine a fresh grape gradually becoming more like a raisin. As the discs lose height, they can't cushion the vertebrae as effectively. This process, called disc degeneration, affects nearly 90% of people by age 50. When discs lose height, it changes the mechanics of your entire spine. The facet joints behind the vertebrae start bearing more weight than they were designed to handle. This can cause these joints to enlarge (a process called facet hypertrophy) and develop arthritis (that’s right, similar to the arthritis in your knee and hip). The ligaments that support your spine, particularly one called the ligamentum flavum, may thicken in response to these changes. For women, menopause brings an additional challenge. The decline in estrogen accelerates bone loss (osteoporosis) and can speed up disc degeneration. This is why vertebral fractures and disc problems are particularly common in women over 60.
How These Changes Cause Pain
Understanding where your pain comes from can be complex because many spinal structures can generate pain signals. Here are the most common sources: Disc-related pain occurs when the outer ring of a disc develops tears or when the gel-like center bulges out (a herniated disc). These changes can cause pain directly in your back or, if the disc presses on a nerve, pain that radiates down your leg (sciatica). Facet joint pain develops when these small joints become arthritic or inflamed. This typically causes pain in your lower back that may spread to your hips or upper thighs. It often feels worse when you stand for long periods or arch your back. Spinal stenosis is a narrowing of the spaces where nerves travel through your spine. This happens when enlarged facet joints, thickened ligaments, and bulging discs all combine to squeeze the spinal canal. The hallmark symptom is leg pain or heaviness that comes on with walking and improves when you sit down or lean forward—a condition called neurogenic claudication. Muscle and ligament strain can occur when the supporting structures of your spine become overworked trying to compensate for weakened discs and joints.
The Good News
While these changes are a normal part of aging, they don't automatically mean you're destined for chronic pain. In fact, many people have significant degenerative changes on imaging studies but experience little to no pain. The relationship between what shows up on an MRI and what you actually feel is surprisingly weak. Moreover, many of the risk factors for back pain are modifiable. Maintaining a healthy weight, staying physically active (particularly with exercises that strengthen your core muscles), not smoking, and managing stress can all reduce your risk of developing disabling back pain. For women in particular, ensuring adequate calcium and vitamin D intake and discussing bone health with your doctor can help prevent vertebral fractures.
When to Seek Help
Most back pain improves on its own within a few weeks. However, you should contact your healthcare provider if you experience: Progressive weakness of one or both legs, difficulty controlling your bladder or bowels, numbness in your private areas, unexplained weight loss, pain that worsens at night or doesn't improve with rest, and/or fever along with back pain.
Understanding your spine's anatomy and how it changes with age empowers you to be an active participant in your care. While aging brings inevitable changes to your spine, knowledge, preventive strategies, and appropriate treatment can help you maintain an active, fulfilling life.
Looking to better understand your back? Take a PostureBackNeck Assessment today.
About the Author:
Rob Turk, MD, MBA
Chief Medical Advisor, MyBackHub
Rob Turk is the Chief Medical Advisor for MyBackHub, Inc. Dr. Turk has a broad foundation of talent in both medicine and business, previously obtaining his MD at the University of California, San Diego School of Medicine and his MBA at the University of Virginia Darden School of Business. As an entrepreneur and orthopaedic spine surgeon, he has unique and valuable insight on many topics. He is a published author in leading scientific journals such as JBJS and Arthroscopy, has written multiple book chapters, and has been a reviewer for a number of scientific journals. He is passionate about motion preservation and innovation in spine care, health equity, delicious food, and sports.
Disclaimer:
As a service to our readers, MyBackHub provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.